Procedures
Offered
Procedures Offered

Dr. Rahul Seth
Dr. Rahul Seth is an experienced, double-board certified facial plastic and reconstructive surgeon. He specializes in surgeries of facial aesthetics and rejuvenation, rhinoplasty and nasal airway breathing, facial reconstruction from skin cancer, craniofacial skeletal and soft tissue trauma, treatment of facial paralysis, and gender-affirming facial surgery. His expertise also includes head and neck free flap tissue transfer, a reconstructive microvascular surgery technique for transplanting tissue from one part of the body to another.
“A positive transformation can have a very meaningful effect on any person. My objective is to be your personal ambassador who provides you that positive and natural change or transformation.”
– Rahul Seth, MD
Our Team
Our Team
Our dedicated team of highly trained professionals help patients achieve their aesthetic goals, while educating them about their treatments and outcomes.
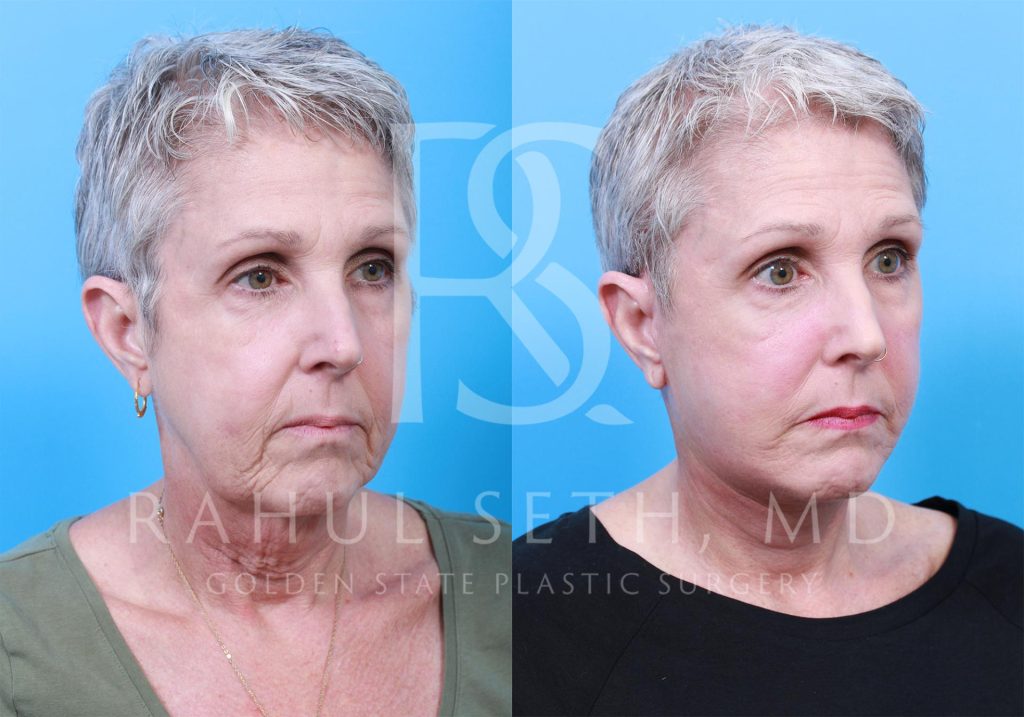
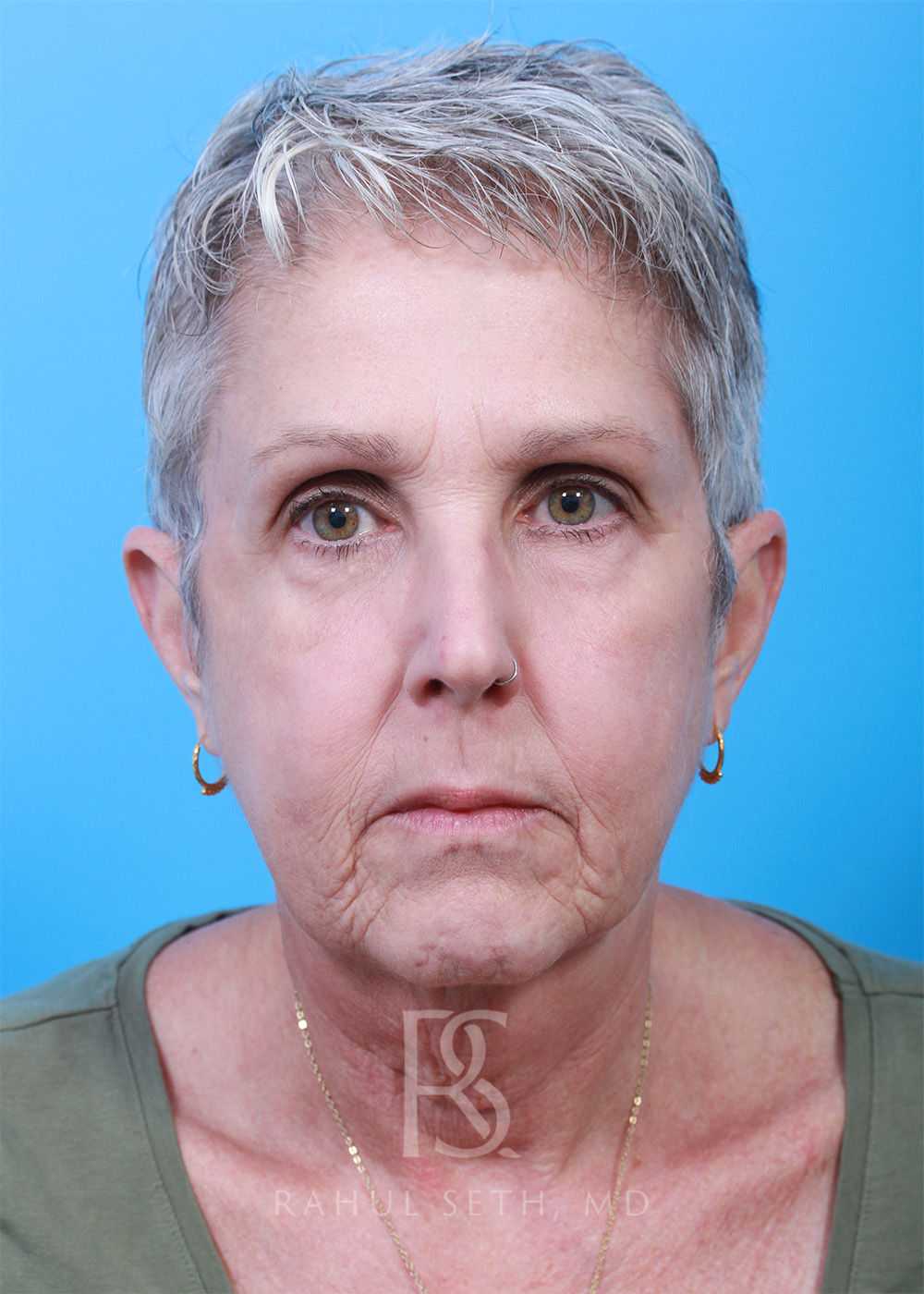
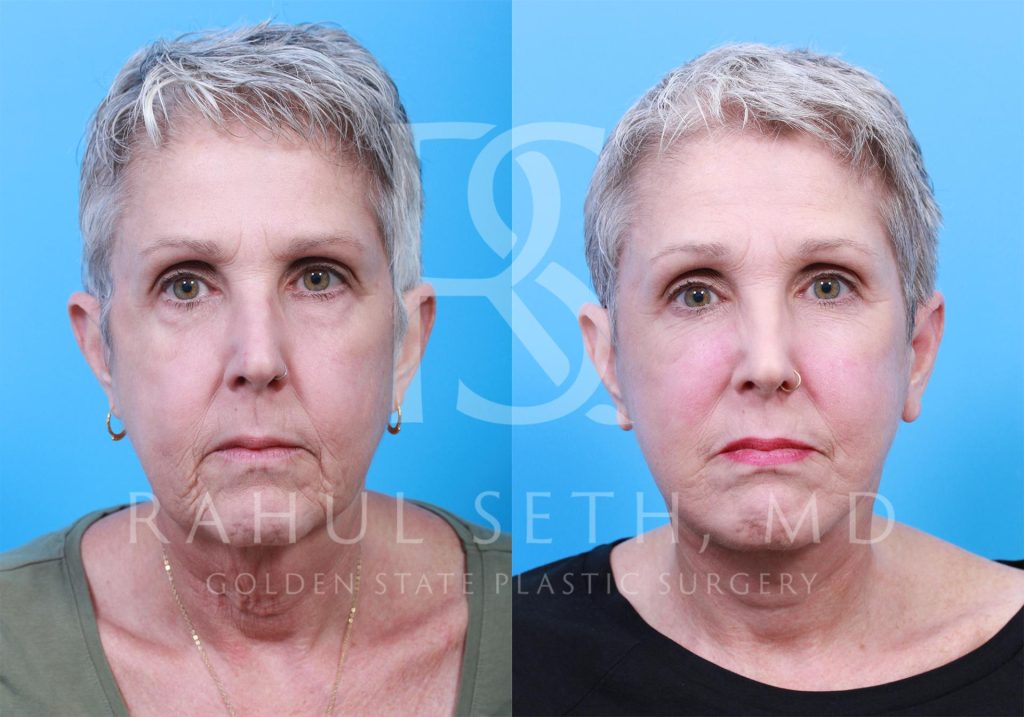
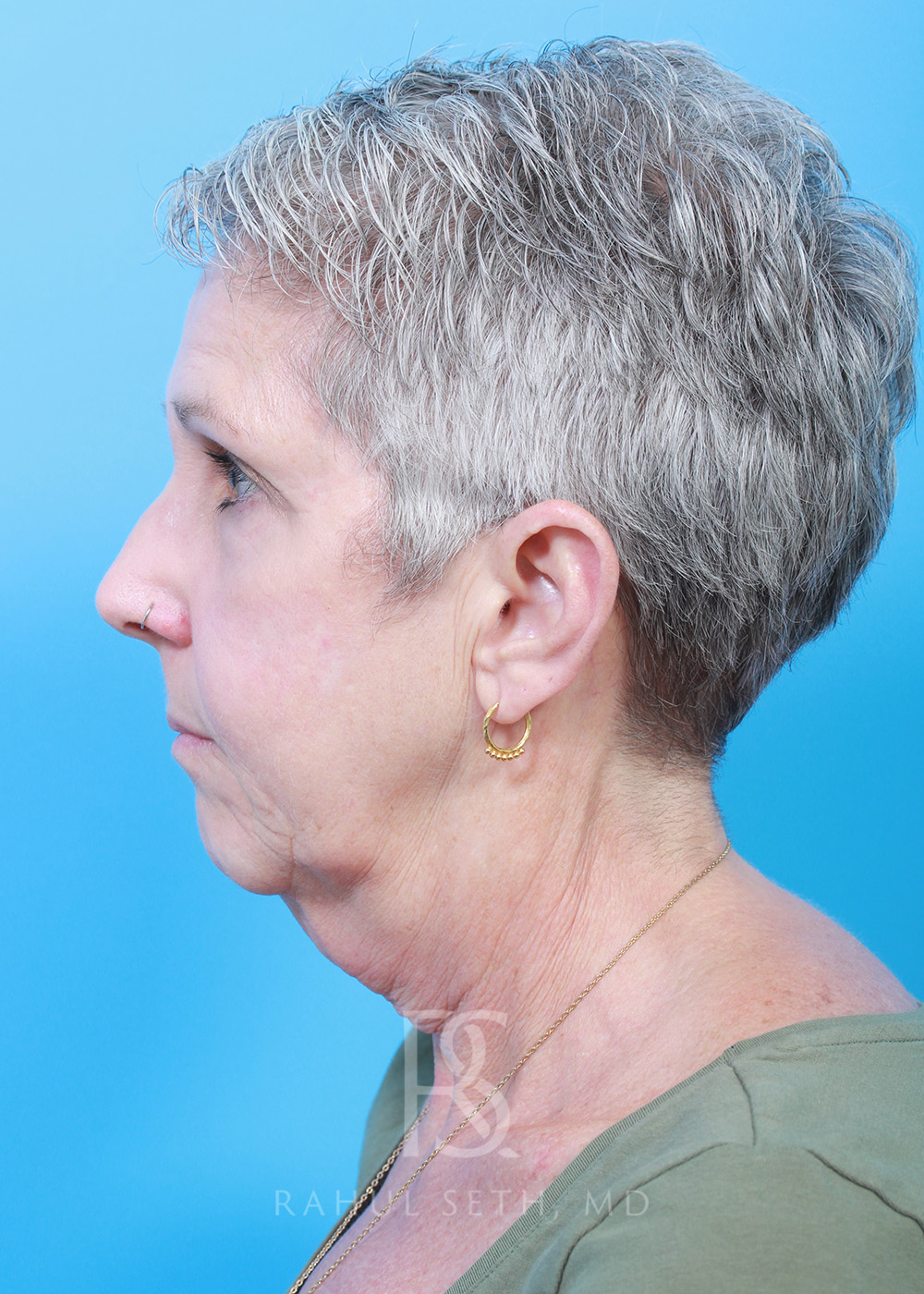
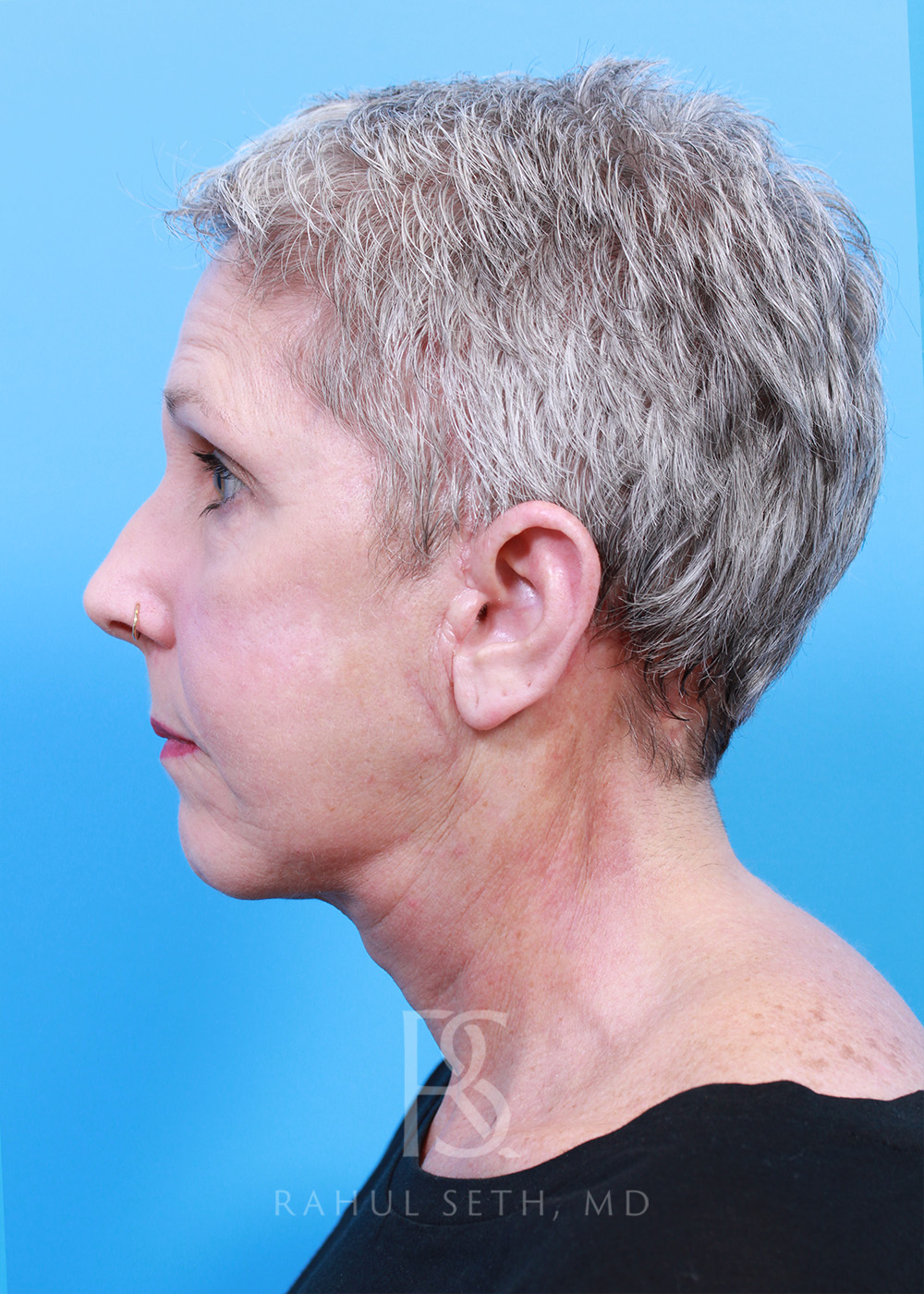
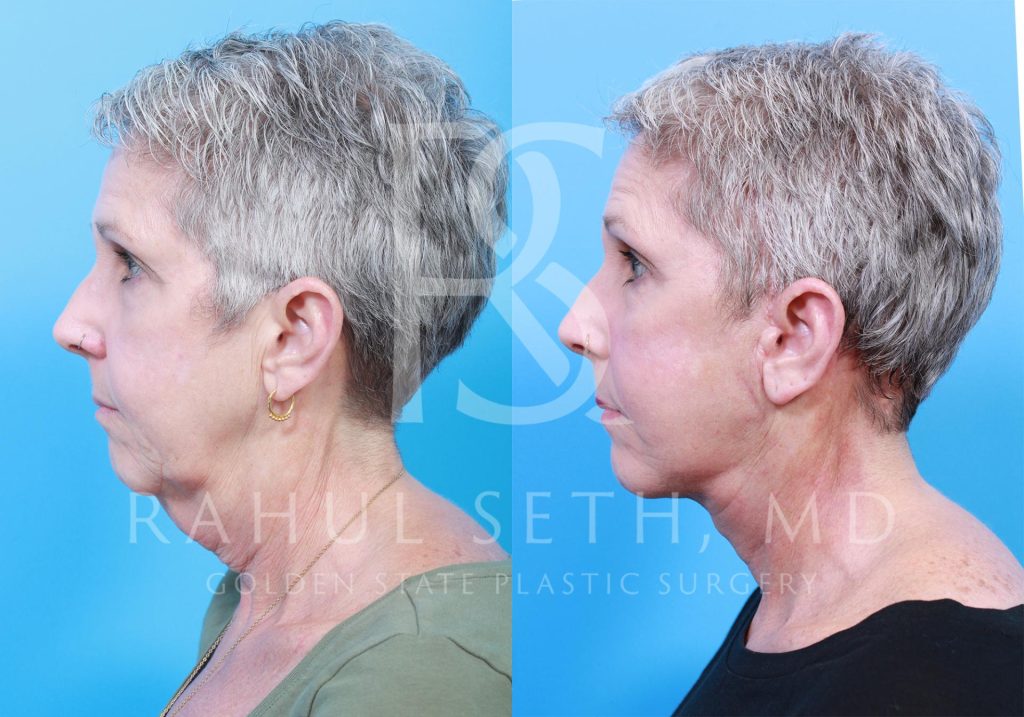
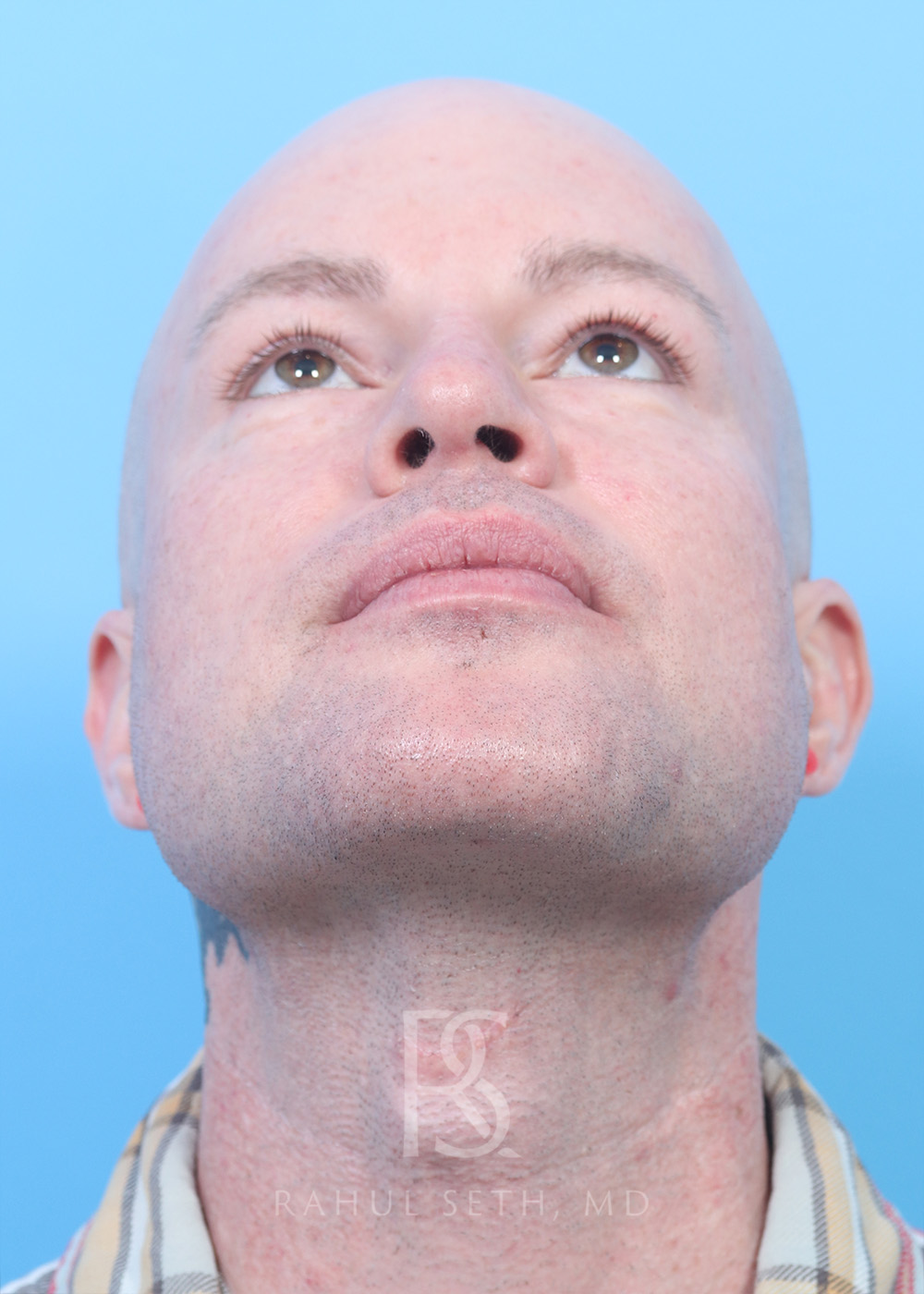
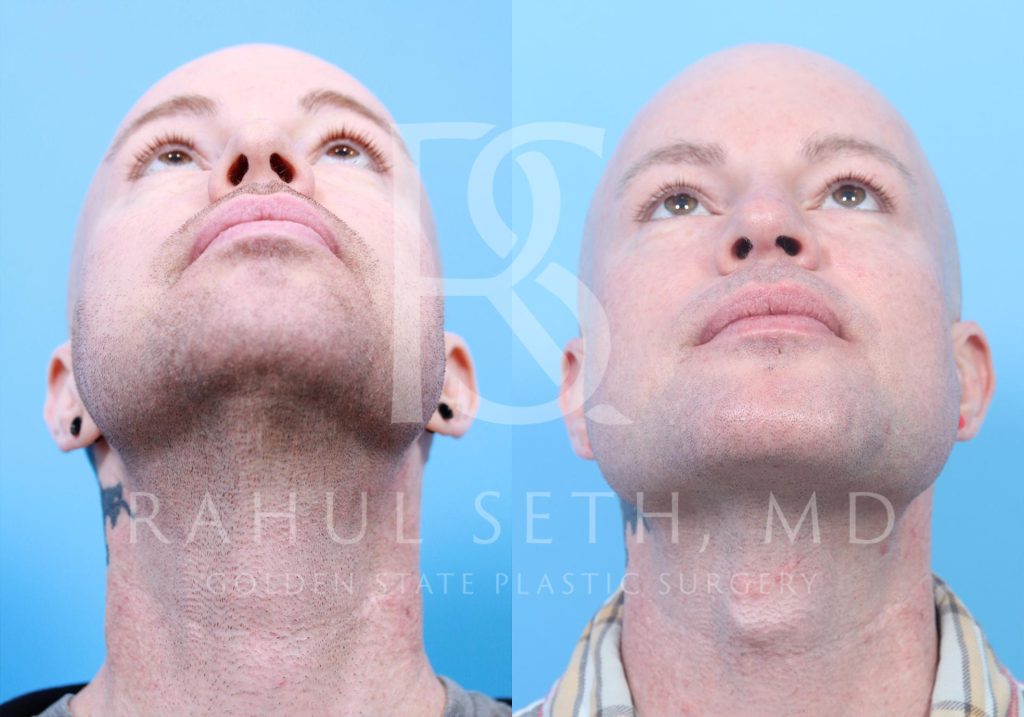
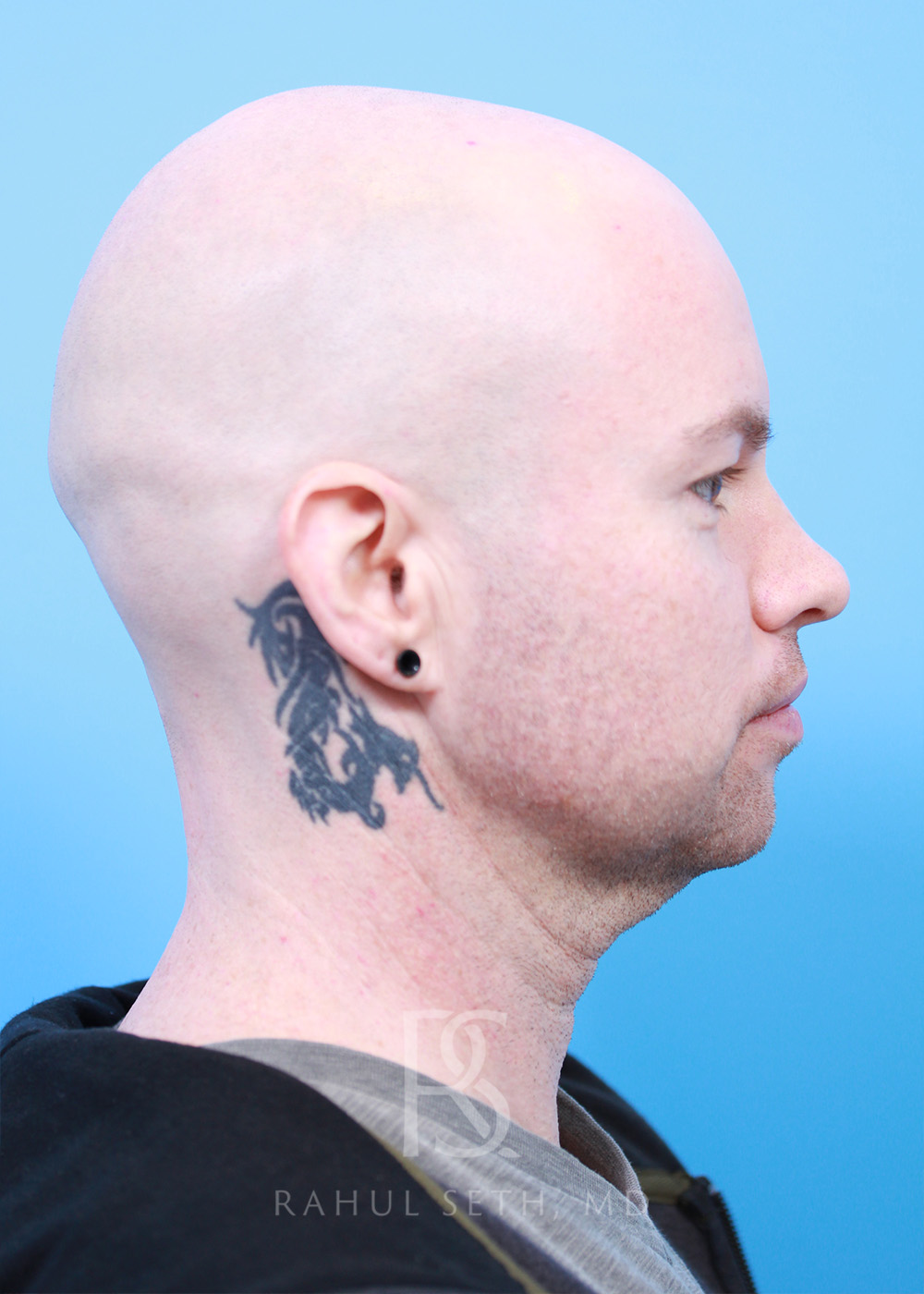
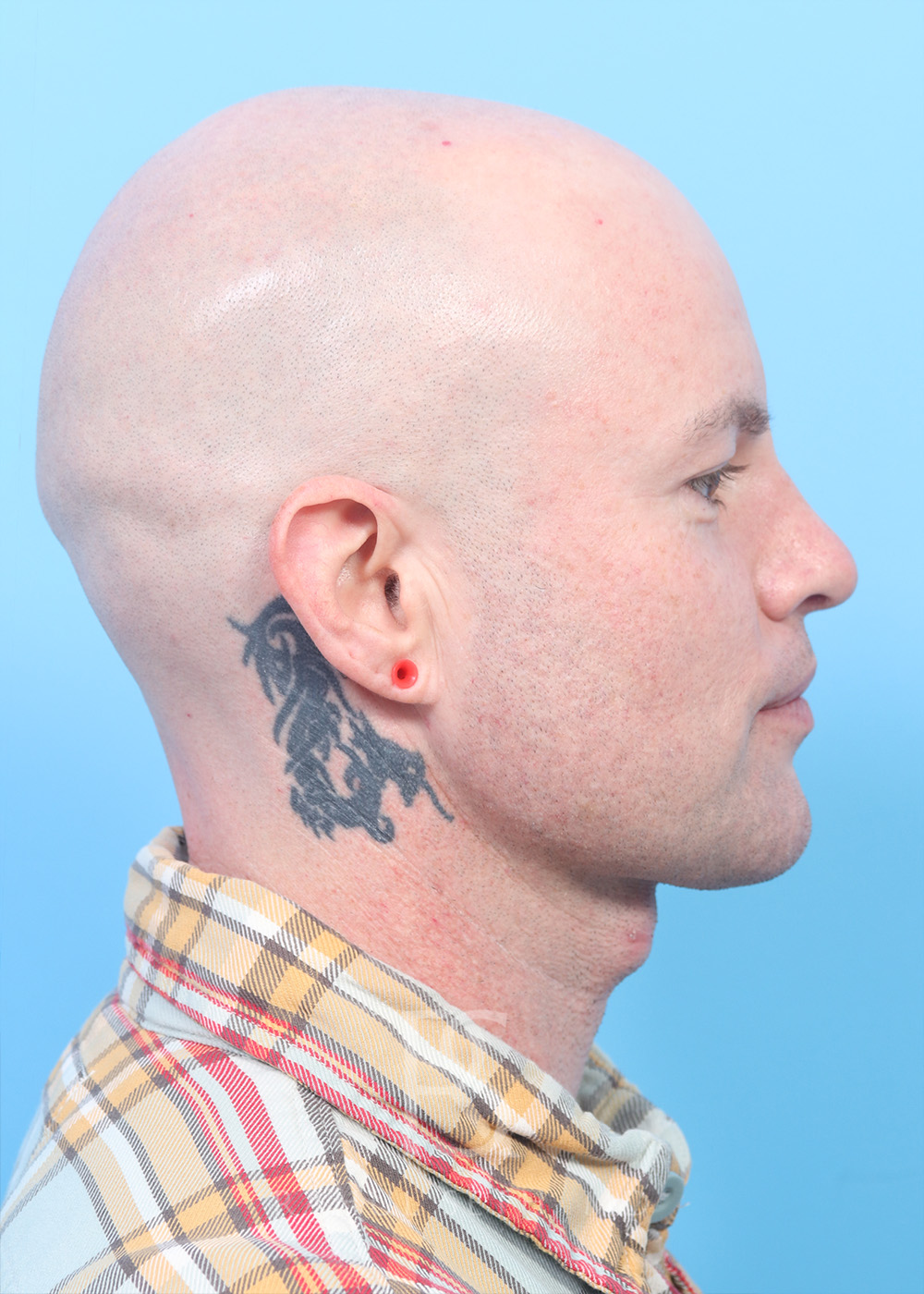
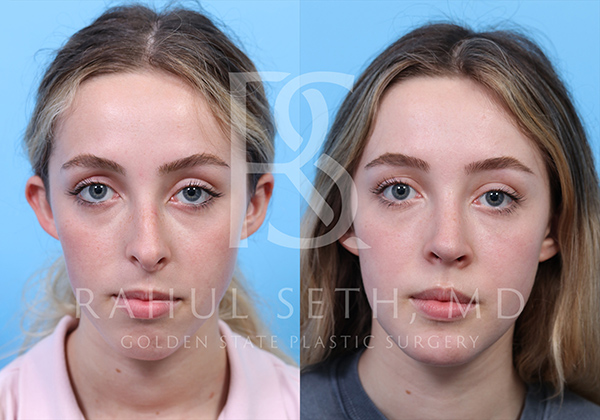
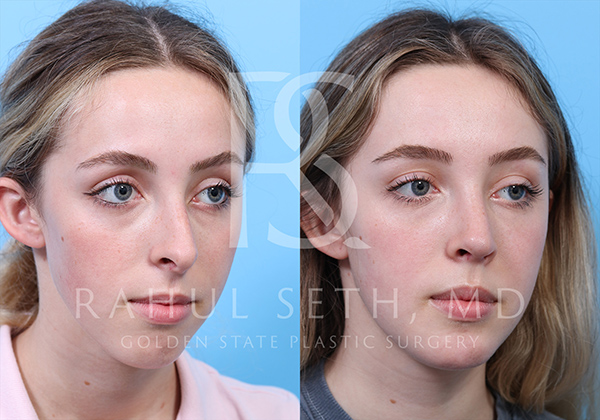
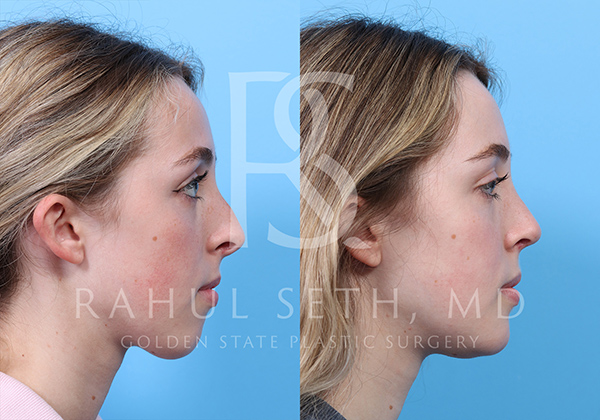
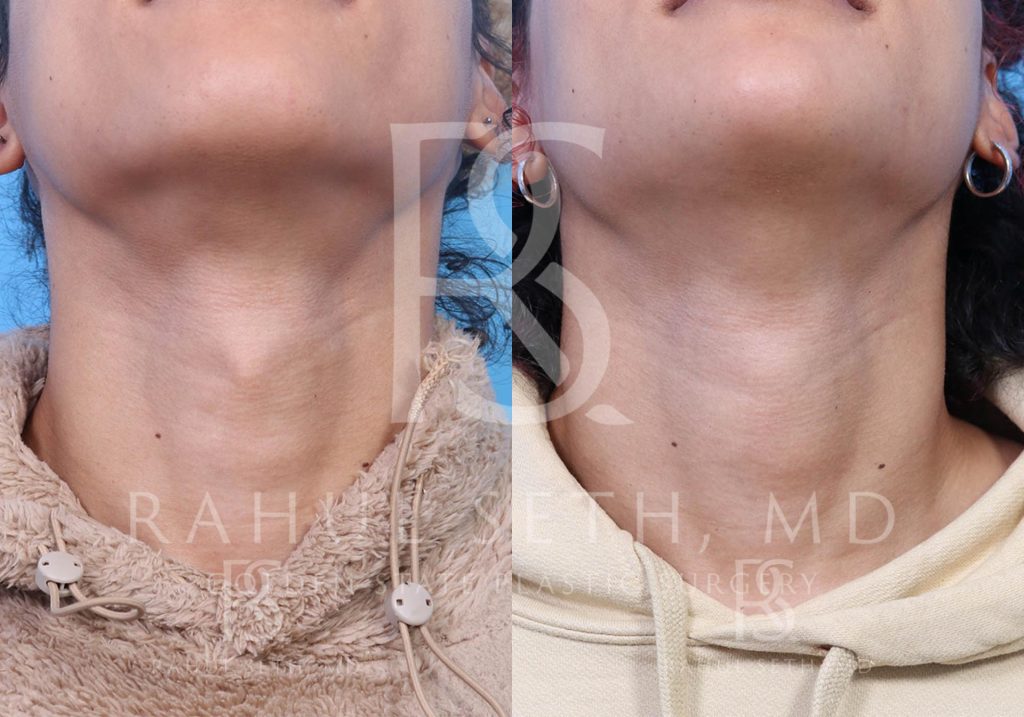
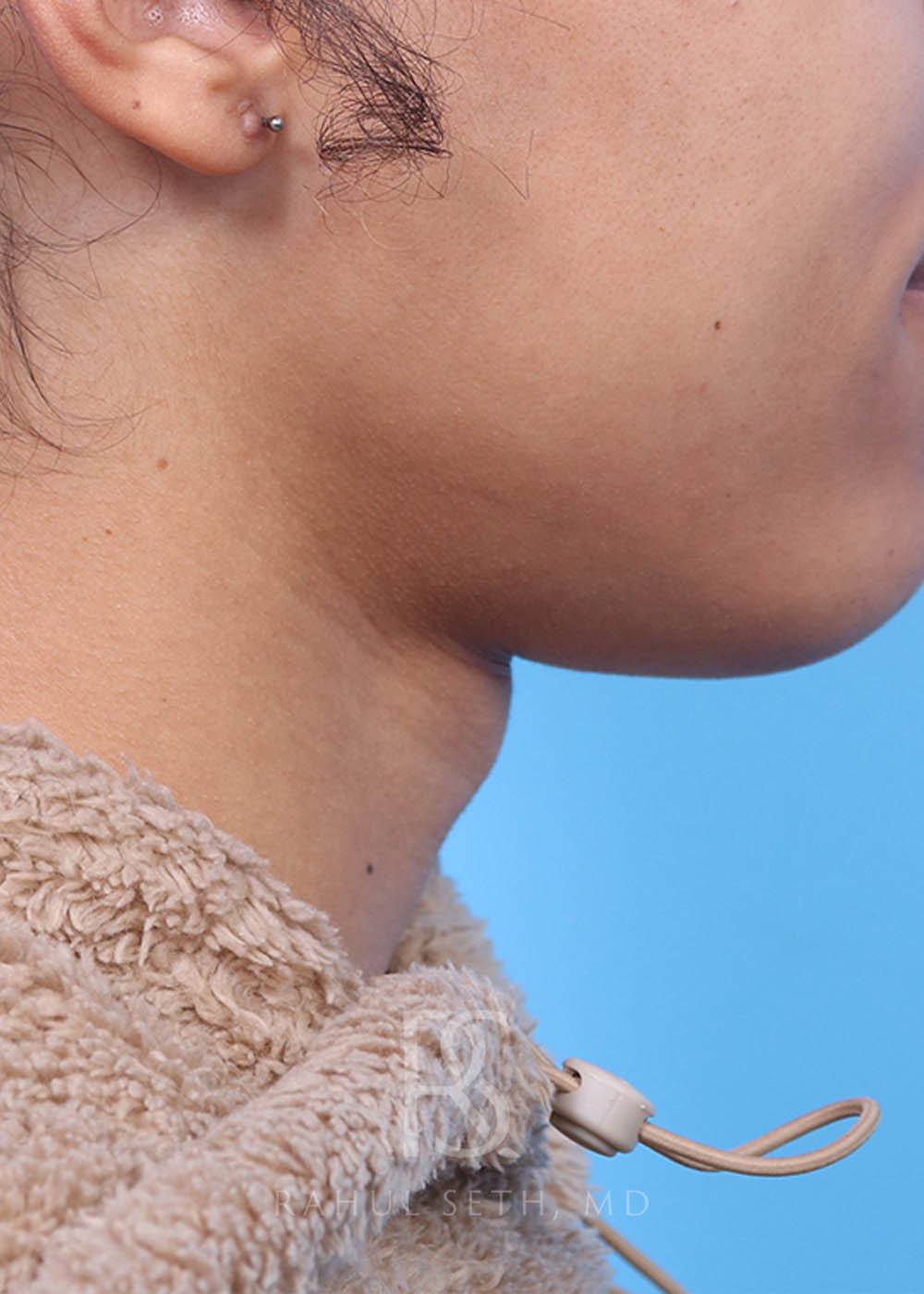
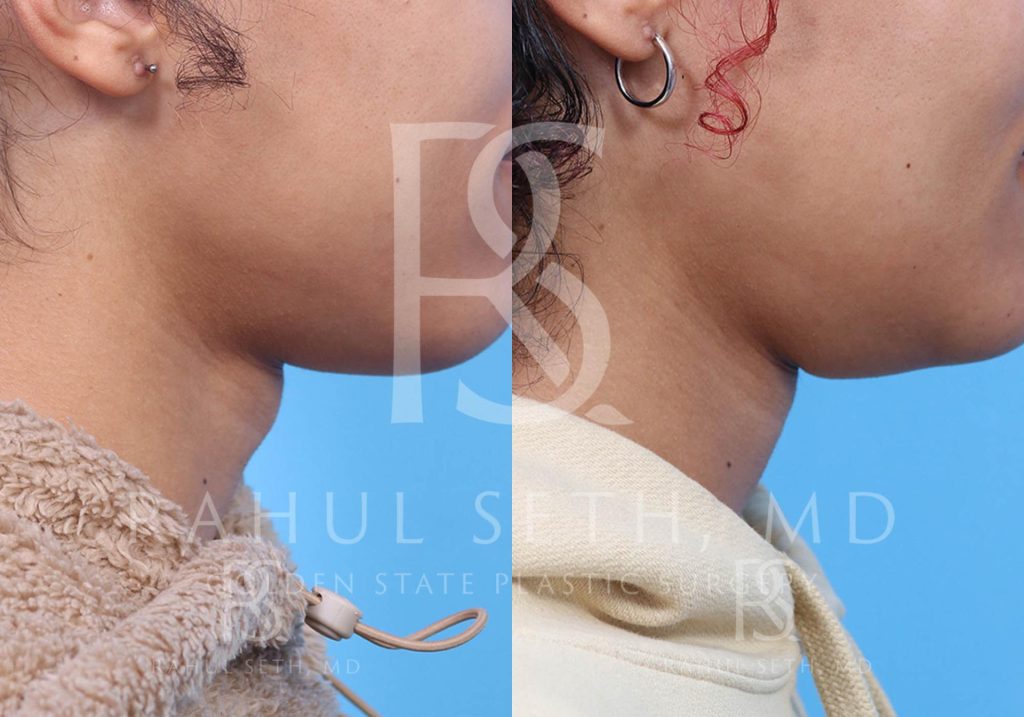
Before & After
Before & After
Testimonials
Testimonials